Influenza
Influenza
Route of infection
Seasonal influenza is highly contagious and is transmitted from person to person. It is transmitted by droplets or by inhaling virus-containing particles that a sick person releases into the air when coughing or sneezing. If viruses get onto a surface, they can also lead to infection through hand contact with the pathogen and subsequent contact with the mucous membranes. Viruses can also spread indirectly by shaking hands, hugging or touching objects that are touched by many people.
Symptomatology
Infections with seasonal influenza can range from asymptomatic (30-50%) to severe or even fatal courses of the disease. Influenza can present with a sudden onset of illness with fever from 38.5 °C, chills, cough and muscle and/or headaches. Mild courses of an upper respiratory tract infection without fever can also occur. Many symptoms of influenza are similar to the symptoms of a common cold (flu-like infection), which can be caused by many other viruses. In the case of true influenza, however, severe and longer-lasting courses occur more frequently. However, this disease can only be differentiated by laboratory detection of influenza viruses.
Therapy
For patients with an uncomplicated influenza infection, treatment focuses on alleviating the symptoms, e.g. with antipyretic painkillers and bed rest. Patients with a severe illness or impaired immune defences can be treated with antiviral medication if an influenza virus infection is confirmed.
Prevention
The most important and effective preventive measure against the disease is the annual flu vaccination. As influenza virus variants can change rapidly, the vaccination must be adjusted every year and thus refreshed seasonally to ensure optimum protection. An annual vaccination is recommended for all people aged 6 months and over. It is particularly important for people over the age of 60 and young children, as well as for people with weakened immune systems such as the chronically ill, pregnant women and overweight people. Vaccination is also particularly recommended for people who live in communal facilities or who come into contact with many people in their work and leisure time.
In addition to the vaccination, hygiene measures can help protect against infection. These include frequent and thorough hand washing, coughing or sneezing into the crook of your arm, throwing away used tissues and regular ventilation. Touching the mucous membranes of the mouth, nose and eyes should be avoided as far as possible. In addition, wearing particle-filtering face masks can help to protect yourself and others from infection with influenza viruses. It is important to limit contact with other people as much as possible if you have symptoms of the disease or to wear a mask if contact is absolutely necessary (e.g. when visiting the doctor in the waiting room). It is possible that you may still be contagious even after the symptoms have subsided.
In Austria, the annual flu season continues throughout the winter months. Flu outbreaks of varying intensity occur regularly. Several systems are used in Austria to monitor the flu situation. The current flu season started in calendar week (CW) 40/2025. Increasing detections of influenza viruses throughout Austria signal the start of the flu epidemic in week 50.
The SARI dashboard shows inpatient admissions to Austrian hospitals with diagnoses of severe acute respiratory infections (SARI). These include influenza (flu), COVID-19, RSV and other severe respiratory diseases.
Since 19 November 2025, AGES has been the new National Reference Centre for Wastewater Monitoring on behalf of the Ministry of Health. The wastewater monitoring dashboard provides current data on the detection of influenza viruses in municipal wastewater samples samples.
Data source for Figs. 1 and 2: The estimated ILI rate per 100,000 inhabitants is an estimate based on data from the City of Vienna’s Municipal Authority 15 influenza information system, ILI reports from Tyrol, and Department 7 of the City of Graz.
Data source for Fig. 3: Eligible insured persons of the ÖGB Health Insurance Fund: employees, PD, KBG, ILI reports from Tyrol
Data source for Tables 4 and 5: Virological sentinel surveillance system (DINÖ): National Reference Laboratory for Influenza, Department of Virology; Medical University of Vienna; Virological non-sentinel surveillance system: Section for Virology, Department of Hygiene, Microbiology and Social Medicine; Medical University IBK, Tyrol; Department of Virology & Infectious Serology, Institute for Hygiene, Microbiology and Environmental Medicine, Medical University of Graz, Styria; Microbiology Laboratory & Group Practice for Travel Medicine, IBK, Tyrol; Analyse BioLab GmbH, Elisabethinen Linz, Upper Austria; SALK Labor GmbH, Salzburg; Institute for Medical Microbiology and Hygiene at Wels-Grieskirchen Hospital, Upper Austria
The Austrian Reference Center for Influenza Epidemiology at the Institute of Medical Microbiology and Hygiene Vienna is responsible for recording the epidemiological situation of influenza in Austria on the basis of a clinical and a virological sentinel surveillance system as well as laboratory reports of influenza virus detections from a further six virological laboratories.
At weekly intervals, the estimated weekly incidence of ILI (influenza like illness) is calculated and published on the AGES homepage Influenza since the beginning of the 2009/2010 season. The data originate from the sentinel ILI surveillance system established since 1992/1993, which consists of the influenza information system of Magistrate 15 of the City of Vienna and the influenza information system of Dept. 7 of the City of Graz (until the 2021/2022 season also the influenza surveillance system Greater Innsbruck). Since the beginning of 2012, ILI case data from the influenza information systems have been processed once a week by the Reference Center for Influenza Epidemiology and sent to the Federal Ministry of Labor, Social Affairs, Health, Care and Consumer Protection (BMASGPK) for transmission to TESSy (The European Surveillance System) and from TESSy to WHO/EuroFlu.
Clinical surveillance
In 1992/93, the ILI (influenza-like illness) sentinel system was established: 52 registered volunteer reporting physicians (general practitioners and pediatricians) of the influenza information systems of Magistrate 15 of the City of Vienna and Dept. 7 of the city of Graz (until 2021/2022 also the influenza surveillance system from the Innsbruck area) report weekly the cases of ILI identified within one working week according to the definition of influenza-like illness (ILI) to the Reference Center for Influenza Epidemiology. Here, the estimated incidence per calendar week is calculated at weekly intervals (number of reported cases per number of inhabitants of the patient catchment area of the reporting physicians).
Virological surveillance
Virological surveillance is performed by the virological sentinel system DINÖ (Diagnostic Influenza Network Austria), coordinated by the National Reference Laboratory for Influenza Viruses at the Center for Virology of the Medical University of Vienna. 98 sentinel physicians (= reporting physicians) send weekly nasopharyngeal swabs of ILI cases to the National Reference Laboratory for Influenza for testing. The weekly number of specimens tested for influenza and the number of those with influenza virus detection are sent by the National Reference Laboratory to the Reference Center for Influenza Epidemiology.
Another five influenza diagnosing laboratories (Section of Virology, Dep. of Hygiene, Microbiology, Social Medicine; Med. University IBK, Tyrol, Department of Virology; Infectious Serology, Institute of Hygiene, Microbiology, and Environmental Medicine; Medical University Graz, Microbiology Laboratory; Joint Practice for Travel Medicine, IBK, Tyrol, Analyse BioLab GmbH; Companies of Elisabethinen Linz and AGES, Upper Austria, SALK Labor GmbH, Salzburg) also report once a week the weekly number of samples with influenza virus detection by virus type or subtype as well as the number of samples tested for influenza. Subtyping of circulating influenza viruses performed by the National Reference Laboratory detects the emergence of new influenza virus variants and allows comparison with strains included in the current vaccine. The aim of the Austrian influenza surveillance system is to monitor influenza activity in order to detect seasonal as well as inter-seasonal influenza epidemics at an early stage.
Excess mortality
The Austrian cause of death statistics are based on death certificates, on which influenza and other respiratory diseases are often not cited as the cause, but rather the complications of an influenza infection or chronic pre-existing conditions that increase the risk of a severe or fatal course. For this reason, it is an international standard that deaths associated with respiratory diseases are estimated by modelling.
Until 2020, the focus was primarily on influenza, as it was the dominant respiratory disease in the winter months. A corresponding model was established in Austria in cooperation between the National Reference Centre for Influenza Epidemiology at AGES (Data Science and Modelling Department) and the National Reference Laboratory for Influenza at the Department of Virology at the Medical University of Vienna (Prof. Dr Theresia Popow-Kraupp; Dr Monika Redlberger-Fritz).
Since the beginning of 2020, SARS-CoV-2 has also been circulating in the winter months. It was therefore necessary to adapt the previously used model in order to avoid overestimating influenza-associated excess mortality and to correct for the circulation of SARS-CoV-2 in addition to extreme temperatures. A basic description of the model is available from Nielsen et al [1]. In order to take into account differences in the lethality of SARS-CoV-2 variants, different dominant variants (wild type, alpha, delta, omicron) were modelled separately.
With the end of the COVID-19 reporting obligation (30 June 2023), the model was adapted again to also estimate COVID-19-associated deaths. As there are no longer any mandatory case reports, the model now relies more heavily on surveillance data from other sources, such as wastewater data and secondary use of electronic health data on hospital admissions due to severe acute respiratory infections (SARI), in order to quantify COVID-19-related mortality.
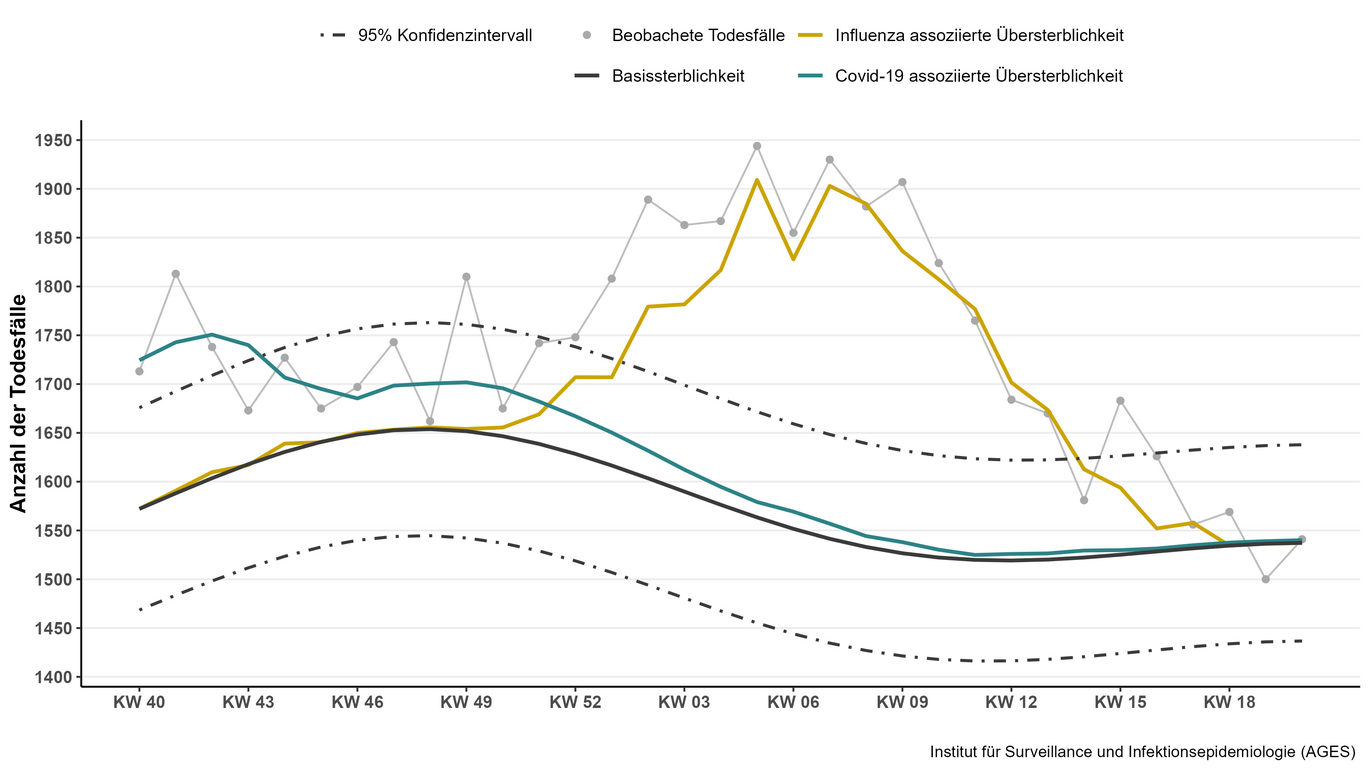
From the 2023/2024 season onwards, the model is based on a negative-binomial regression analysis in which the total population is taken into account as the reference variable. Indicators for the circulation of specific respiratory pathogens (influenza, SARS-CoV-2) and extreme weather events such as hot or cold spells are included as explanatory variables. In addition, harmonic terms are used to adequately reflect seasonal fluctuations in baseline mortality. This model structure enables a differentiated estimate of excess mortality caused by influenza and COVID-19 infections, taking into account seasonal, demographic and temperature-related influencing factors.
It should be noted that the estimates relate exclusively to the period between calendar week 40 and calendar week 20, i.e. the typical weeks of the influenza season.
| Season | WEEK | Estimated number of deaths associated with influenza (95% CI) |
|---|---|---|
| 2015/2016 | 40-20 | 492 (207; 777) |
| 2016/2017 | 40-20 | 4.939 (4.585; 5.292) |
| 2017/2018 | 40-20 | 4.277 (3.920; 4.633) |
| 2018/2019 | 40-20 | 2.022 (1.748; 2.296) |
| 2019/2020 | 40-20 | 1.714 (1.431; 1.998) |
| 2020/2021 | 40-20 | 0 |
| 2021/2022 | 40-20 | 652 (215; 1.089) |
| 2022/2023 | 40-20 | 4.020 (3.578; 4.462) |
| 2023/2024 | 40-20 | 2.696 (2.593; 2.798) |
| 2024/2025 | 40-20 | 3.570 (3.452; 3.688) |
Data sources
Deaths in Austria (excluding deaths abroad) from 2000 by calendar week: Statistics Austria - data.statistik.gv.at(open.data from Statistics Austria).
Weekly influenza positive rate: virological sentinel surveillance system, DINÖ, Diagnostic Influenza Network Austria
Weekly ILI incidence: clinical sentinel surveillance system, operated at the National Reference Centre for Influenza Epidemiology, AGES
National surveillance data for SARS-CoV-2
Inpatient admissions in Austrian hospitals with diagnoses of Severe Acute Respiratory Infections (SARI) - www.sari-dashboard.at
COVID-19 wastewater indicator for Austria as a whole - abwassermonitoring.at
Temperature data for Austria: GeoSphere Austria - dataset.api.hub.geosphere.at
References
1 Nielsen J, Rod NH, Vestergaard LS, Lange T. Estimates of mortality attributable to COVID-19: a statistical model for monitoring COVID-19 and seasonal influenza, Denmark, spring 2020. Eurosurveillance. 2021; doi:10.2807/1560-7917.ES.2021.26.8.2001646
2 Nielsen J, Krause TG, Mølbak K. Influenza-associated mortality determined from all-cause mortality, Denmark 2010/11-2016/17: The FluMOMO model. Influenza Other Respir Viruses. 2018; doi:10.1111/irv.12564
Contact
Nationale Referenzzentrale für Influenzaepidemiologie
- infektionsepidemiologie@ages.at
- +43 50 555 37111
-
Währingerstraße 25a
1090 Wien
Last updated: 17.04.2026
automatically translated