Corona virus
SARS-CoV-2
Pathogen reservoir
Various domestic, pet, and wild/zoo animal species, such as felines (including large cats such as tigers, lions, etc.), dogs, ferrets, tanuki, deer, golden hamsters, rabbits, and various primates (e.g., gorillas) can be infected with SARS-CoV-2. In all known cases of natural infection, it most likely occurred via infected humans. The severity of clinical signs ranges from asymptomatic to mild clinical signs, depending on the species affected (primarily felines and ferrets, as well as minks); according to current knowledge, animals play no role in the spread of infection. An exception is mink from commercial fur farms, where infection of exposed humans has been documented.
Currently, it is not considered necessary or advisable to separate from pets in case of infection of humans or animals.
Infection route
Transmission of SARS-CoV-2 occurs mainly via virus-containing particles that are excreted, for example, when infectious persons speak loudly, sing, or cough or sneeze. Aerosols (finest airborne liquid particles) and droplets play a crucial role in this process. Aerosols can remain suspended in the air for prolonged periods of time and disperse in inadequately ventilated indoor spaces, leading to infection.
The relative risk of environmental SARS-CoV-2 transmission through contaminated surfaces is considered low compared with direct contact, droplet transmission, or airborne transmission.
Symptomatology
The symptomatology of SARS-CoV-2 infections depends in its duration, frequency, and severity on the circulating variant, among other factors. The most common symptoms observed to date include: Fever, chills, and sore throat. Also common are cough, difficulty breathing, general symptoms such as fatigue and aching limbs, loss of smell and taste, nausea and vomiting, dizziness, and difficulty sleeping.
In more severe cases, the infection causes severe shortness of breath (at rest or when speaking), confusion, drowsiness or loss of consciousness, chest pain or pressure, and pale to bluish skin color, among other symptoms. Severe courses can lead to death.
There are also asymptomatic courses.
Infections with SARS-CoV-2 can have long-term consequences. A distinction is made between long-COVID and post-COVID (see the technical information). The symptoms can be of a physical and/or psychological nature. Frequently, a so-called "fatigue" is reported by those affected.
This list does not contain all possible symptoms, the course can be very different (see technical information). The symptoms vary depending on the SARS-CoV-2 variant and the immune status of the affected person.
Therapy
Treatment of mildly symptomatic patients without risk factors for a severe course is basically symptomatic, i.e., by alleviating the symptoms of the disease, e.g., by administering antipyretics.
For high-risk patients and patients with a severe course, various pharmaceutical agents are available (e.g., paxlovide, veklury, or corticosteroids).
The use of antibiotics is not recommended (unless there is a bacterial superinfection), as antibiotics are not effective against SARS-CoV-2.
Prevention
Vaccination, depending on the circulating variant and the timing and level of immunization, partially protects against infection and, in particular, against severe courses and death.
To protect against infection, it is recommended that hands be washed with soap and water or disinfected with an alcohol-based disinfectant several times a day. It is also recommended to ventilate indoor areas regularly and spend time outdoors whenever possible. To minimize the risk of infection, in addition to vaccination, WHO advises continuing to keep your distance and wearing a well-fitting mask if distance is not possible and the room is poorly ventilated. As a general rule, when sneezing, it is always advised to cover the mouth and nose with a cloth or bent elbow, not the hands.
These preventive measures generally reduce the risk of colds and are especially recommended when infection or hospitalization rates increase.
If symptoms appear, it is advised to stay at home and avoid contact.
Situation in Austria
By 30 June 2023, 6,084,529 cases had been reported in Austria. The graph on the development of the 7-day incidence shows the course of the pandemic from 28 February 2020. The peak of the 7-day incidence was reached in March 2022, with the most cases reported in one day on 15 March 2022 (63,468). Since 30 June 2023, COVID-19 is no longer a notifiable disease in Austria.
The SARI dashboard shows inpatient admissions to Austrian hospitals with diagnoses of Severe Acute Respiratory Infections (SARI). These include COVID-19, influenza, RSV and other severe respiratory diseases.
Since 19 November 2025, AGES has been the new National Reference Centre for Wastewater Monitoring on behalf of the Ministry of Health. The dashboard provides current data on the detection of SARS-CoV-2 in municipal wastewater samples available.
Excess mortality
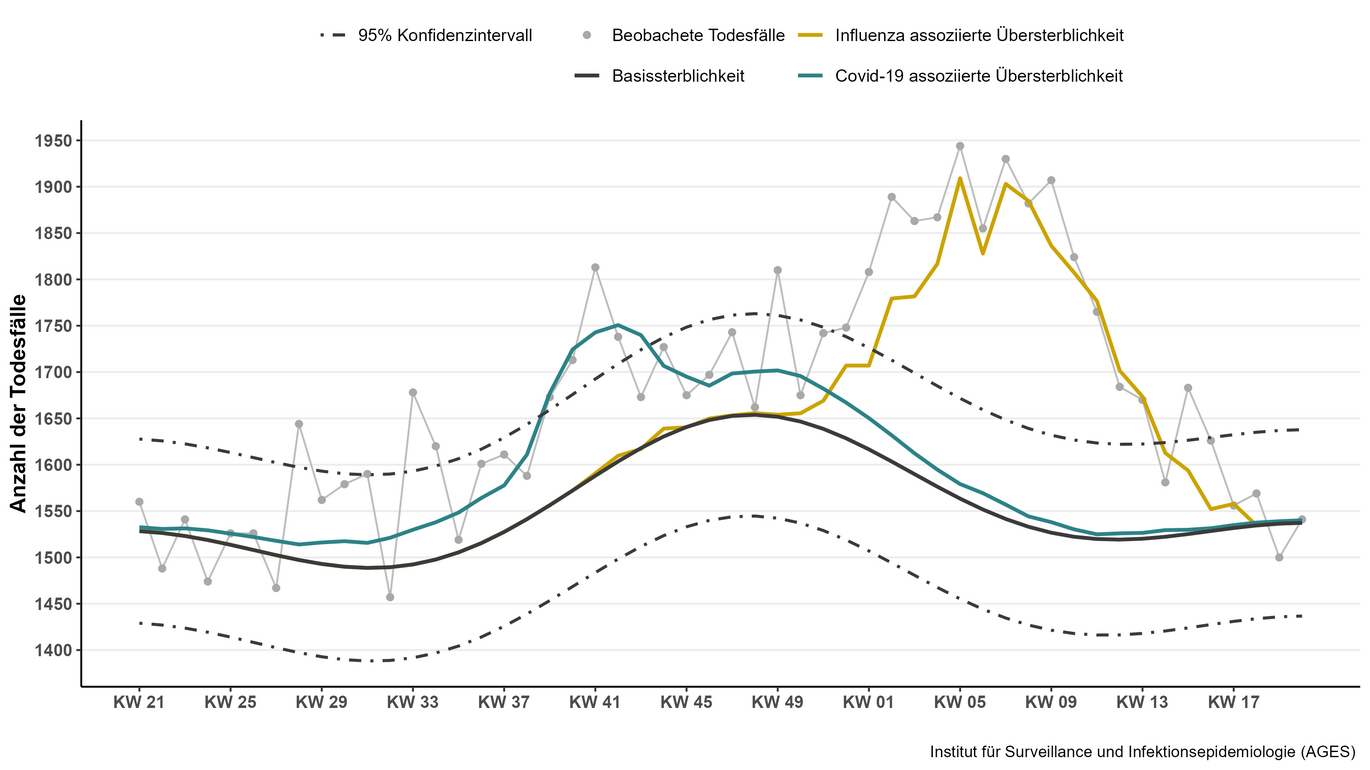
With the end of the mandatory reporting of SARS-CoV-2 infections on 30 June 2023, the basis for direct recording of COVID-19 deaths in Austria no longer applies. In the Austrian cause of death statistics based on death certificates, Covid-19 and other respiratory diseases are often not mentioned as a cause, but rather complications or chronic pre-existing conditions that increase the risk of a severe or fatal course. Nevertheless, in order to be able to assess the impact of SARS-CoV-2 on mortality, it was necessary to establish a model-based estimate of excess mortality for COVID-19.
The model is based on the model developed for estimating influenza-associated excess mortality. Based on this, a step-by-step extension was made that takes into account the circulation of SARS-CoV-2 and thus enables simultaneous estimation of influenza- and COVID-19-associated excess mortality. Since the abolition of mandatory reporting, the model has increasingly relied on data from alternative surveillance systems, such as wastewater monitoring and secondary use of electronic health data on hospital admissions due to severe acute respiratory infections (SARI), to quantify COVID-19-related mortality.
While the typical season for influenza is defined as calendar week 40 to calendar week 20 of the following year, the period from calendar week 21 to calendar week 20 of the following year is shown for COVID-19, the epidemic occurrence of which does not yet follow a specific seasonal pattern. This enables potential seasonal patterns to be recorded throughout the year and a differentiated assessment of the excess mortality caused by COVID-19.
Table 1: Estimated number of deaths associated with SARS-CoV-2 infections (calendar week 21 to calendar week 20 of the following year), including 95% confidence interval (CI), Austria.
| Season | CALENDAR WEEK | Estimated number of deaths associated with Covid-19 (95 % CI) |
| 2023/2024 | 21-20 | 2.512 (2.413; 2.611) |
| 2024/2025 | 21-20 | 1.849 (1.764; 1.935) |
Data sources
Deaths in Austria (excluding deaths abroad) from 2000 by calendar week: Statistics Austria - data.statistik.gv.at(open.data from Statistics Austria).
Weekly influenza positive rate: virological sentinel surveillance system, DINÖ, Diagnostic Influenza Network Austria
Weekly ILI incidence: clinical sentinel surveillance system, operated at the National Reference Centre for Influenza Epidemiology, AGES
National surveillance data for SARS-CoV-2
Inpatient admissions in Austrian hospitals with diagnoses of Severe Acute Respiratory Infections (SARI) - www.sari-dashboard.at
COVID-19 wastewater indicator for Austria as a whole - abwassermonitoring.at
Temperature data for Austria: GeoSphere Austria - dataset.api.hub.geosphere.at
References
1 Nielsen J, Rod NH, Vestergaard LS, Lange T. Estimates of mortality attributable to COVID-19: a statistical model for monitoring COVID-19 and seasonal influenza, Denmark, spring 2020. Eurosurveillance. 2021; doi:10.2807/1560-7917.ES.2021.26.8.2001646
2 Nielsen J, Krause TG, Mølbak K. Influenza-associated mortality determined from all-cause mortality, Denmark 2010/11-2016/17: The FluMOMO model. Influenza Other Respir Viruses. 2018; doi:10.1111/irv.12564
Variants in Austria
AGES carried out whole genome sequencing of SARS-CoV-2-positive samples until 20 June 2024 in order to break down the spread of known variants and discover new SARS-CoV-2 variants. Due to the low number of SARS-CoV-2 samples for sequencing, these analyses have been paused for the time being.
A detailed breakdown of the SARS-CoV-2 variants registered between the beginning of July 2023 and June 2024 can be found in the .csv file at the bottom of the page under "Downloads".
Further information can be found on the dashboard of the national wastewater monitoring programme.
International variants
The SARS-CoV-2 variants are categorised by the ECDC and the WHO into different categories, depending on how their characteristics and further development are assessed: Variant of Concern (VOC), Variant of Interest (VOI) and Variant under Monitoring (VUM).
No variant is currently considered to be a Variant of Concern.
On 24 January 2025, the WHO added LP.8.1 as a "Variant under Monitoring".
An overview of the exact classifications can be found in the table below.
According to the latest monthly COVID-19 update from the WHO dated 17 January 2025, XEC was the most common SARS-CoV-2 variant worldwide in December with a prevalence of approx. 38.6 %. KP.3.1.1 has decreased in prevalence and now accounts for 33.2% of sequencing worldwide.
The most common SARS-CoV-2 variants in Europe in the third week of January were XEC (58%), KP.3.1.1 (12%), KP.3.1 (8 %), JN.1 (5 %) and JN.1.11 (4 %), JN.1.16.1 (3 %), JN.1.16 (3 %), KP.1.1 (2 %) and KP.3 (2 %).
The weekly updates of the variants are discontinued, significant developments can be found monthly in the AGES radar for infectious diseases.
Mutations repeatedly lead to a line splitting into several, slightly different lines. These are known as sublines. They are often given their own names and numbers, which means that the relationship is not always obvious (as in the case of subline JN.1, which belongs to BA.2.86, see legend).
Legend:
VOC = Variant of Concern
VOI = Variant of Interest
VUM = Variant under Monitoring
* = Variant including associated sublines
BA.2.86 = B.1.1.529.2.86
JN.1 = BA.2.86 + S:L455S
KP.2 = JN.1 + S:R346T, S:F456L, S:V1104L
KP.3 = JN.1 + S:F456L, S:Q493E, S:V1104L
KP.3.1.1 = KP.3 + S:S31-
KP.3.1.1 = KP.3 + S:S31-
JN.1.18 = JN.1 + S:R346T
LB.1 = JN.1 + S:S31-, S:Q183H, S:R346T, S:F456L
XEC = KS.1.1 + KP.3.3
Specialized information
Symptomatology
Via entry into cells through the ACE2 receptor, manifestations are possible in all tissues where these receptors are present; the type and severity of manifestation depends, among other things, on the density of the receptors. In addition, in some cases there are exaggerated immune reactions and circulatory disturbances as a result of increased blood clotting.
Pulmonary manifestations are very common. In addition to colds, pneumonia can develop during the course of the disease, which can subsequently turn into Acute Respiratory Syndrome (ARDS). This may necessitate extracorporeal oxygen saturation by ECMO.
Neurologically, COVID-19 may manifest neuropsychiatrically in addition to headache, dizziness, and confusion; strokes, (meningo) encephalopathies, Guillain-Barré and Miller-Fisher syndromes also occur.
Cardiovascularly, myocardial damage, myocarditis, acute myocardial infarction, heart failure, cardiac arrhythmias, and various thromboembolic events resulting from the infection have been described.
Especially in severely ill COVID-19 patients, renal failure (requiring dialysis) may occur.
If hyperinflammatory syndromes occur, damage to various organs occurs as a consequence (multi-organ failure). The mortality is high(RKI - Coronavirus SARS-CoV-2 - Hyperinflammation Syndrome in COVID-19 (27.07.2020)).
Co-infections frequently occur, including with Mycoplasma pneumoniae, Candida albicans, and Aspergillus spp.
Known risk factors for a severe course include: Hypertension, diabetes mellitus, chronic liver and kidney damage, coronary artery disease, COPD (chronic obstructive pulmonary disease), cerebrovascular disease, regular use of immunosuppressive drugs, cancer, obesity, arrhythmias, and ischemic heart disease(see ECDC).
Infections with SARS-CoV-2 may involve long-term sequelae. A distinction is made between long-COVID and post-COVID. Long-COVID is when symptoms that occurred during the confirmed infection persist for more than four weeks after the onset of illness. Symptoms that do not appear until twelve weeks after the onset of the disease or reappear, persist for at least two months, and cannot be explained in any other way are referred to as post-COVID. The symptoms can be of a physical and/or psychological nature. Fatigue is frequently reported by those affected, as well as shortness of breath, concentration and memory problems, sleep disturbances, muscle weakness and muscle pain.
Therapy
The current therapy recommendations for the treatment of an infection with SARS-CoV-2 can be found here:
RKI - Coronavirus SARS-CoV-2 - COVID-19: Therapy notes and recommendations
Diagnostic
Diagnosis of infection with SARS-CoV-2 is made by means of a secretion obtained from the upper respiratory tract, for example by means of a mouth or nasopharyngeal swab. Samples should be taken as close as possible to the onset of symptoms. The samples obtained can be used to perform rapid antigen tests, for which the result is usually available within ten to 30 minutes. The most reliable detection method is PCR testing for SARS-CoV-2 RNA. Saliva samples can also be examined by PCR; antigen tests are too unspecific here.
In hospitalized patients, secretions from the lower respiratory tract can be obtained for PCR diagnosis.
Blood tests for the detection of SARS-CoV-2 antibodies can detect infections that have already occurred, but are not important for acute diagnostics. The test for antibodies may also be positive as a result of previous vaccination. A negative result does not exclude a previous infection with SARS-CoV-2, as the number of antibodies decreases again with time.
Last updated: 17.04.2026
automatically translated