Tularemia
Francisella tularensis
Infection route
Contact and smear infection or splashes of pathogen-containing fluids (especially when cutting up field hares), but also through tick bites or insect bites. Dust or droplet infection can also occur when skinning or cutting up infected brown hares and when working with agricultural products such as hay, straw, grain, or sugar beets if they are contaminated with mouse excreta or carcasses. Transmission through contaminated food or water is possible.
Symptomatology
In humans, a painless ulcer usually develops at the site of contact. Common symptoms are fever, headache, pain in the limbs, and painful swelling of the regional lymph nodes. There may be varying courses of disease with different symptoms such as pharyngitis, vomiting, diarrhea, or abdominal pain. Diseased brown hares may exhibit unusual movements and lack of flight behavior.
Situation in Austria
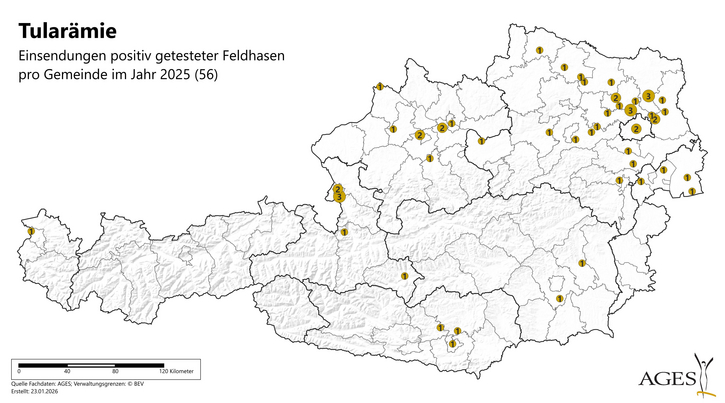
In 2025, 70 cases of the disease were reported in humans in Austria (as of 21 January 2026). In 2025 (as of 26 January 2026), tularemia was confirmed in 56 hares, 29 of which were in Lower Austria, 8 in Upper Austria, 7 in Salzburg, 4 in Burgenland, 3 in Carinthia, 2 each in Styria and Vienna, and 1 in Vorarlberg (see table). Since 2018, endemic tularemia has also been detected in brown hares in western Austria, with frequent submissions of positive hares mainly from Salzburg and Upper Austria. In November 2023, tularemia was detected for the first time in Carinthia in a brown hare.
Specialized information
While Francisella tularensis subspecies holarctica biovar II (erythromycin resistant) is endemically distributed in eastern Europe, biovar I (erythromycin sensitive) of subspecies holarctica is found in western Austria in addition to biovar II. The different distribution areas of biovars I and II in western and eastern Europe, respectively, overlap in western Austria. Rabbits and rodents(Lagomorpha and Rodentia) are considered reservoir animals of tularemia. Ectoparasites, especially ticks, also play an important role in maintaining the natural range as vectors. Francisella tularensis occurs in both dermacentor and Ixodes ricinus ticks. Francisella tularensis subspecies holarctica, which occurs in Europe, North America, and Japan, and subspecies mediaasiatica, which occurs in Central Asia, usually cause less severe, localized disease in humans, whereas life-threatening, generalized forms of disease are possible when infected by the highly virulent subspecies tularensis, which occurs primarily in North America. Transmission occurs by contact and smear infection or splashing of pathogen-containing fluids (especially when cutting up field hares), but also by tick bites or insect bites. Dust or droplet infection may also occur when skinning or cutting up infected brown hares and when working with agricultural products such as hay, straw, grain, or sugar beets if they are contaminated with mouse excreta or carcasses.
Symptomatology
The clinical picture varies greatly depending on the route of transmission and the site of entry of the pathogen. While the ulceroglandular or glandular form with inflammation of the lymph nodes in the upper extremities is usually observed in infection by field hares, the site of entry of the pathogen in transmission by arthropods is more likely to be in the lower extremities. In tick-bite transmission, a punched-out ulcer (Eschar-like) develops around the bite site, followed by regional lymphadenitis (lymphadenitis) and occasionally fever (ulceroglandular form). Aerogenous transmission may result in high-fever pneumonia.
Diseased brown hares may exhibit unusual movements and lack of flight behavior.
Prevention and control
Dead and diseased field hares that have been killed, as well as hares that have been shot with pathological changes in the internal organs, must not be thrown away or buried under any circumstances, but should be sent to the IVET in Mödling for examination or disposed of in a disease-proof manner. Since hares with chronic renal enterolaemia excrete francisella in their urine over a long period of time, hunters in endemic areas should pay increased attention to killing sick animals with unusual behavior in order to prevent further spread of the pathogen. Sick, killed, or dead brown hares should not be skinned, but should be touched only with gloves and immediately packed securely to prevent infection of humans by inhalation of dust containing the pathogen or touching fur, blood, or excretions.
Contact
Institut für veterinärmedizinische Untersuchungen Mödling
- vetmed.moedling@ages.at
- +43 50 555 38112
-
Robert Koch-Gasse 17
2340 Mödling
Last updated: 26.02.2026
automatically translated